Connect With Us
Blog
Items filtered by date: January 2024
Types of Diabetic Wounds
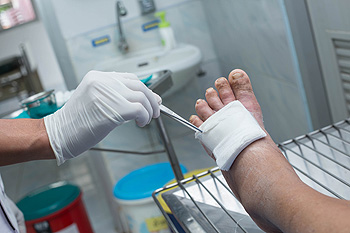
Diabetic wounds are a common complication of diabetes, resulting from neuropathy and vascular disease. Nerve damage diminishes foot sensation, making it challenging to detect an injury. Vascular disease impairs blood flow, which reduces the speed of healing wound. Diabetic foot ulcers are the most prevalent type of wound. They are open sores on pressure points, typically caused by neuropathy, trauma, and pressure. Early detection and treatment are essential to prevent infections and potential limb loss. Diabetic neuropathic wounds stem from nerve damage, leading to a loss of protective sensation. These wounds may appear as calluses, corns, or blisters, requiring specialized care to prevent infections and further damage. Ischemic wounds arise from an inadequate blood supply, often due to peripheral artery disease, or PAD, which is exacerbated by diabetes. Characterized by poor circulation and delayed healing, ischemic wounds pose an increased risk of infection. If you are experiencing frequent or stubborn foot wounds that will not heal properly or seem infected, it is suggested that you seek the help of a podiatrist for care.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with James Torhorst, DPM from Torhorst Foot and Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our offices located in Waupaca and Stevens Point, WI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Do You Suffer From Painful Feet?
Reasons to See a Podiatrist
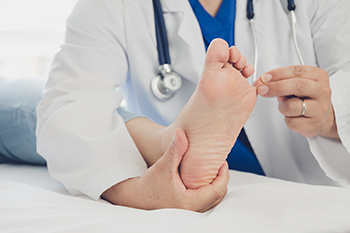
Podiatrists are specialized healthcare professionals who focus on the diagnosis, treatment, and prevention of foot and ankle disorders. There are various compelling reasons to schedule a visit to a podiatrist. First, persistent foot or ankle pain should not be ignored, as it can be an indicator of an underlying issue. Podiatrists are experts in identifying and addressing the source of your discomfort. They can diagnose conditions such as plantar fasciitis, bunions, or heel spurs, and develop personalized treatment plans. If you are experiencing mobility issues, a podiatrist can help. They can provide custom orthotics or recommend appropriate footwear to improve your gait and balance. Diabetes can take a toll on the feet, leading to complications like neuropathy and ulcers. Regular check-ups with a podiatrist are essential for early detection and preventative care. In short, consulting a podiatrist is beneficial for anyone seeking to maintain their overall foot health, in addition to alleviating foot pain. It is suggested that you visit a podiatrist if you are interested in learning more about the field of podiatry.
If you are dealing with pain in your feet and ankles, you may want to seek help from a podiatrist. Feel free to contact James Torhorst, DPM from Torhorst Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Podiatrist?
A podiatrist is a doctor of podiatric medicine who diagnoses and treats conditions of the foot, ankle, and related structures of the leg. Your podiatrist may specialize in a certain field such as sports medicine, wound care, pediatrics, and diabetic care. Podiatrists have the ability to become board certified through training, clinical experience, and then taking an exam.
What Do Podiatrists Do?
On a daily basis, a podiatrist may perform the following activities:
- Diagnose foot ailments such as ulcers, tumors, fractures, etc.
- Use innovative methods to treat conditions
- Use corrective orthotics, casts, and strappings to correct deformities
- Correct walking patterns and balance
- Provide individual consultations to patients
It is very important that you take care of your feet. It’s easy to take having healthy feet for granted, however foot problems tend to be among the most common health conditions. Podiatrists can help diagnose and treat a variety of feet related conditions, so it is crucial that you visit one if you need assistance.
If you have any questions please feel free to contact our offices located in Waupaca and Stevens Point, WI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Definition and Causes of Plantar Fibromas
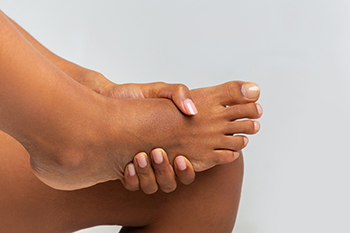
Plantar fibroma, a condition affecting the feet, involves the formation of non-cancerous, fibrous tissue growths within the plantar fascia, which is the ligament spanning the bottom of the foot. These nodules, often slow-growing, manifest as small lumps beneath the skin, leading to discomfort and potential limitations in foot mobility. The exact cause of plantar fibromas remains elusive, but factors such as genetics and trauma to the plantar fascia are considered contributory. The condition tends to be more prevalent in individuals with a family history of plantar fibromas, emphasizing a genetic predisposition. Additionally, repetitive stress or injury to the plantar fascia, often incurred through excessive standing or walking, can trigger the development of these fibrous nodules. Understanding the definition and potential causes of plantar fibroma lays the foundation for informed discussions with podiatrists and the exploration of appropriate management strategies for this relatively common yet nuanced foot condition. If you have these kinds of growths on your feet, it is suggested that you speak with a podiatrist who can correctly diagnose and treat plantar fibromas.
A plantar fibroma may disrupt your daily activities. If you have any concerns, contact James Torhorst, DPM of Torhorst Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Plantar Fibroma
A plantar fibroma is a fibrous knot in the arch of the foot. It is embedded in the plantar fascia which is a band of tissue that extends from the heel to the toes along the bottom of the foot. There can be multiple plantar fibromas in the feet at the same time. There are no known causes for this condition. If you have a plantar fibroma, there will be a bump in the arch of your foot that cannot be missed. Any associated pain is most often due to a shoe rubbing against the nodule. Non-surgical options, such as steroid injections, physical therapy, and orthotics should be tried first. Surgery is a last resort and is the only thing that will remove a plantar fibroma entirely. Consult with a podiatrist for a proper diagnosis and to determine the treatment regimen that is right for you.
What Causes a Plantar Fibroma?
While there are no specific causes identified, a plantar fibroma can possibly come from genetic predisposition or the formation of scar tissue that forms from healing the tears in the plantar fascia.
What Are the Symptoms of a Plantar Fibroma?
There will be a noticeable lump in the arch of the foot that may or may not cause pain. If pain is felt, it is typically because a shoe is rubbing up against the lump or when walking or standing barefoot.
Treatment and Prevention
A plantar fibroma will not disappear without treatment, but it can get smaller and be a non-issue. If pain persists, a podiatrist examines the foot and when the arch of the foot is pressed, pain can be felt down to the toes. An MRI or biopsy might be performed to help diagnose or evaluate the plantar fibroma. The following non-surgical options are generally enough to reduce the size and pain of these nodules:
- Steroid injections
- Orthotics
- Physical therapy to help apply anti-inflammatory creams on the bump
Surgery is considered if the mass increases in size and the patient continues to feel pain after non-surgical methods are tried.
If you have any questions please feel free to contact our offices located in Waupaca and Stevens Point, WI . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Common Causes of Toe Pain
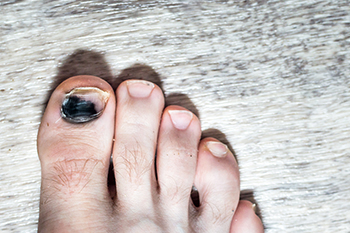
Toe pain is a common discomfort that can significantly impact your daily life. One of the leading causes is wearing shoes that are too tight or too loose, which can exert pressure on the toes, leading to pain and discomfort. Additionally, injuries such as stubbing or dropping heavy objects on the toes can result in acute pain. Ingrown toenails, a condition where the nail grows into the surrounding skin, are another common culprit. Arthritis, characterized by inflammation of the joints, can affect the toes and cause persistent pain. Toe pain may also be indicative of conditions like gout or bunions, where joint inflammation and deformities contribute to discomfort. Understanding these common causes empowers individuals to make informed choices about their footwear, lifestyle, and seek timely medical attention from a podiatrist to alleviate toe pain and enhance overall foot health. If you are experiencing toe pain, it is suggested that you visit this type of doctor who can determine the cause and offer appropriate treatment options.
Toe pain can disrupt your daily activities. If you have any concerns, contact James Torhorst, DPM of Torhorst Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
- Trauma
- Sports injury
- Wearing shoes that are too tight
- Arthritis
- Gout
- Corns and calluses
- Hammertoe
- Bunions
- Blisters
- Ingrown toenails
- Sprains
- Fractures (broken bones)
- Dislocations
When to See a Podiatrist
- Severe pain
- Persistent pain that lasts more than a week
- Signs of infection
- Continued swelling
- Pain that prevents walking
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please feel free to contact our offices located in Waupaca and Stevens Point, WI . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Ways to Reduce Pain From High Heels
Walking in high heels can exude confidence and style, but it often comes at the expense of comfort. To navigate the world of stilettos without enduring pain, consider a few essential tips. First, choose heels with a reasonable height and platform, allowing for better weight distribution. Prioritize proper shoe size to avoid unnecessary pressure on toes and insteps. Engage core muscles for improved balance, maintaining an upright posture to alleviate strain on the lower back. Mastering a heel-to-toe walking technique ensures a smoother gait, reducing impact on the feet. Take smaller steps and embrace a slower pace to enhance stability and grace. Additionally, opt for shoes with cushioned insoles or consider using gel inserts for added comfort. Gradual practice in heels at home can help build endurance and confidence. Lastly, pamper your feet with stretches and massages. If you would like more information about how to wear high heels while protecting the feet, it is suggested that you confer with a podiatrist.
High heels have a history of causing foot and ankle problems. If you have any concerns about your feet or ankles, contact James Torhorst, DPM from Torhorst Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Effects of High Heels on the Feet
High heels are popular shoes among women because of their many styles and societal appeal. Despite this, high heels can still cause many health problems if worn too frequently.
Which Parts of My Body Will Be Affected by High Heels?
- Ankle Joints
- Achilles Tendon – May shorten and stiffen with prolonged wear
- Balls of the Feet
- Knees – Heels cause the knees to bend constantly, creating stress on them
- Back – They decrease the spine’s ability to absorb shock, which may lead to back pain. The vertebrae of the lower back may compress.
What Kinds of Foot Problems Can Develop from Wearing High Heels?
- Corns
- Calluses
- Hammertoe
- Bunions
- Morton’s Neuroma
- Plantar Fasciitis
How Can I Still Wear High Heels and Maintain Foot Health?
If you want to wear high heeled shoes, make sure that you are not wearing them every day, as this will help prevent long term physical problems. Try wearing thicker heels as opposed to stilettos to distribute weight more evenly across the feet. Always make sure you are wearing the proper shoes for the right occasion, such as sneakers for exercising. If you walk to work, try carrying your heels with you and changing into them once you arrive at work. Adding inserts to your heels can help cushion your feet and absorb shock. Full foot inserts or metatarsal pads are available.
If you have any questions please feel free to contact our offices located in Waupaca and Stevens Point, WI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

